
Learn common causes of severe night sweats, warning signs, medical workup, menopause options, and practical cooling solutions for better sleep.
Severe night sweats can do more than ruin a night of sleep. They can soak clothing and sheets, raise stress, worsen fatigue, and sometimes point to a medical problem that needs attention. Across top search results from AAFP, ACOG, The Menopause Society, Cleveland Clinic, and the CDC, the message is consistent, the real challenge is separating simple overheating from causes like menopause, medication effects, infection, sleep apnea, thyroid disease, or, less often, cancer. Good care usually combines two things, symptom relief that helps tonight, and a workup that explains why this is happening in the first place.
Yes. Severe night sweats with fever, weight loss, swollen lymph nodes, or a new cough need prompt medical evaluation. The AAFP and CDC both treat these patterns seriously because infections, lymphoma, tuberculosis, endocrine disease, and medication reactions can look like ordinary overheating at first.
A mild warm spell is not the same thing as severe night sweats. In practice, severe usually means you are repeatedly waking up drenched, changing sleepwear, changing sheets, or losing sleep because your body feels intensely hot or clammy. If that is happening often, it deserves attention.
The biggest red flags are pretty straightforward. If your sweats come with unplanned weight loss, measured fever, swollen glands in the neck or armpits, persistent cough, easy bruising, chest pain, or new shortness of breath, do not rely on cooling tricks alone. Common misconception, many people assume drenching night sweats are “just hormones,” but infections and blood related cancers can present that way too.
If you already know you are in perimenopause or menopause, that history matters, but it does not erase the need for a proper review if the pattern changes suddenly or becomes extreme.
Several causes are common. Menopause, SSRIs, prednisone, obstructive sleep apnea, hyperthyroidism, and infections sit near the top of the list in primary care. Cleveland Clinic and AAFP guidance both emphasize that severe night sweats are a symptom cluster, not a diagnosis by themselves.
For adults, the most common buckets are hormonal shifts, medicines, sleep disorders, infections, endocrine conditions, and lifestyle triggers. Menopause and perimenopause are major drivers of vasomotor symptoms, meaning the brain and blood vessels trigger heat release and sweating even when the room is not especially warm.
Medication effects are easy to miss. SSRIs, SNRIs, corticosteroids, thyroid hormone, some blood pressure medicines, opioids, diabetes medicines, and stimulant drugs can all contribute. If your sweats began after starting or changing a medicine, that timing matters.
Then there are medical causes that need a different path. If you snore loudly, wake gasping, or feel unrefreshed, obstructive sleep apnea moves higher on the list. If you have tremor, palpitations, weight loss, or heat intolerance all day, hyperthyroidism becomes more plausible. If you wake shaky or hungry, especially with diabetes treatment, low blood sugar may be part of the picture.
Alcohol, anxiety, spicy meals late at night, and a bedroom that is simply too warm can worsen any of the above. If the room is hot and the bedding traps heat, symptoms often get louder, but that still does not mean the room caused the whole problem.
The best home plan starts with direct cooling, trigger control, and medical review. A bFan bed fan, a medication check, and tighter sleep temperature control can reduce symptom burden quickly, while you sort out the cause. Home steps help most when they support, not replace, diagnosis.

If you want the biggest return from simple changes, start with measures that directly move heat away from your skin and keep the room in a sleep friendly range.
Start with history, then basic testing, then targeted follow up. A primary care clinician or gynecologist usually begins with medication review, fever and weight checks, and focused labs. If clues point to sleep apnea, thyroid disease, infection, or cancer, testing gets more specific.
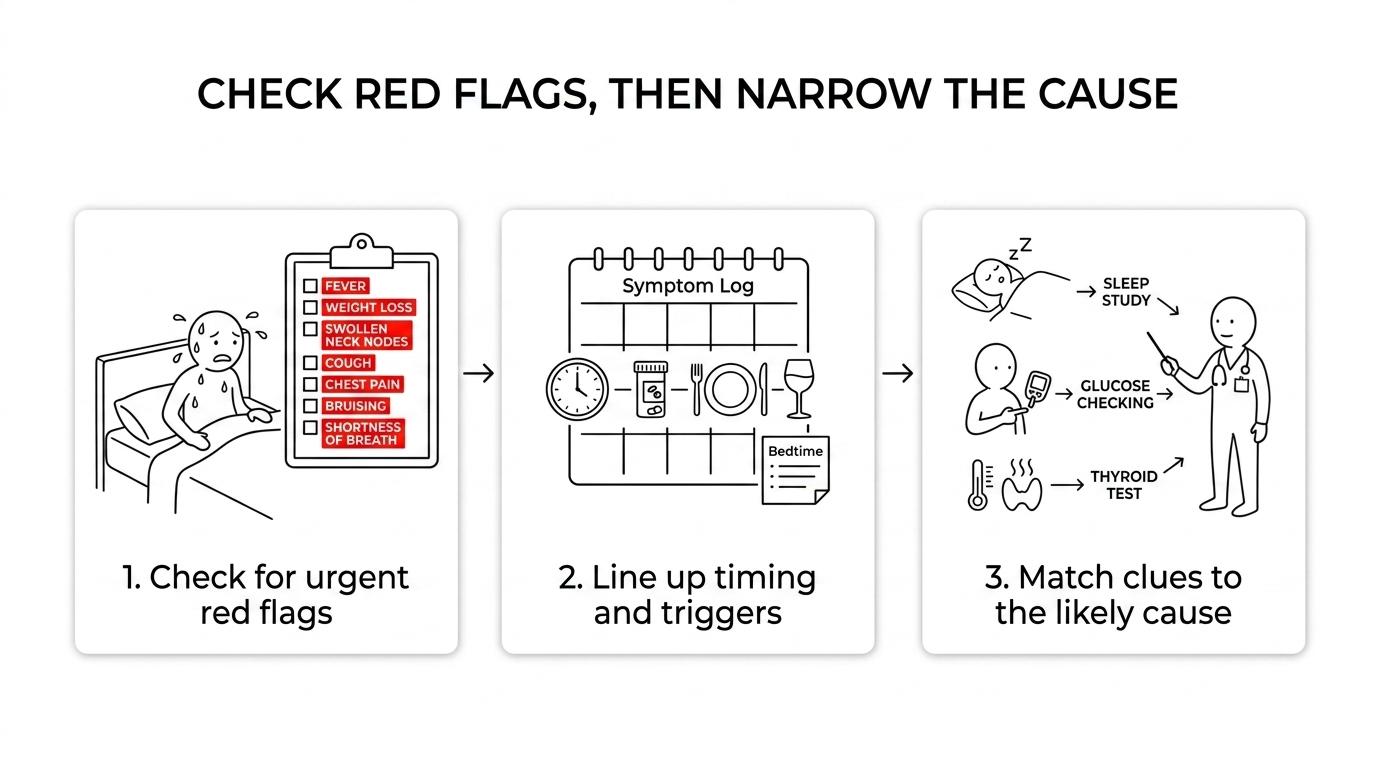
Step 1 is the story. When did the sweats start, how often do they happen, how wet do you get, and what else is happening with them? A clinician will usually ask about menopause symptoms, recent infections, travel, snoring, anxiety, alcohol, and any recent medication changes.
Step 2 is basic screening. Common first tests may include a complete blood count, thyroid testing, glucose testing, and sometimes inflammatory markers, based on symptoms. If you have daytime symptoms too, that may push the workup beyond a simple sleep problem.
Step 3 is targeted testing. If you have cough, fever, or exposure risk, then infection testing or chest imaging may follow. If you snore heavily or stop breathing during sleep, then a sleep study may make sense. If lymph nodes are enlarged or weight loss is real and unplanned, then more urgent imaging or specialist referral is appropriate.
A good rule is simple, if the story is clearly linked to perimenopause or a new medicine, the path may be relatively direct. If the pattern is unexplained, getting drenching, or joined by red flags, the workup should move faster.
Hormone therapy is usually the most effective option. ACOG and The Menopause Society both place systemic hormone therapy first for eligible patients with moderate to severe menopausal vasomotor symptoms. Fezolinetant, SSRIs, SNRIs, gabapentin, and CBT are valid alternatives when hormones are not the right fit.
The trade off is that the best symptom control is not always the safest or simplest choice for every person. If you have a uterus, estrogen usually needs a progestogen partner. If you have certain clotting, cancer, liver, or cardiovascular risks, nonhormonal options may be safer.
After that high level decision, the differences get more practical.
Bed microclimate control works best when you cool the space inside the bedding, not just the whole room. A bFan, tight weave sheets, and a smart thermostat setting can make a major difference because trapped heat around the torso and legs is often the real problem.
Step 1 is to set the room sensibly. Sleep experts commonly recommend about 60°F to 67°F for better sleep. If you use a Bedfan, many people can keep the room roughly 5°F warmer and still feel cool enough to sleep, which can trim AC use without sacrificing comfort.
Step 2 is to set airflow under the covers, not across your face. Place the bed fan near the foot of the bed so it sends room air between the sheets. This is exactly where systems shown on bfan.world focus, and it is why tight weave sheets usually perform better than very loose knits.
Step 3 is to let timing do some of the work. The first half of the night often needs more cooling than the last part, so timer controls can help you avoid waking up chilly at 3 a.m. Pro tip, people often overcool the whole room when targeted airflow would have done the job with less energy.
A common misconception needs clearing up here. Neither Bedfan nor BedJet cools the air itself. They use the cooler air already in the room and move it through the bed so your body can release heat more effectively.
A bFan is usually the better value for direct airflow cooling. BedJet and bFan both use room air, not refrigerated air, but BedJet costs much more, while lowering central AC cools the whole room and usually costs more to run. Cost, noise, control, and partner needs drive the choice.
This is where trade offs matter more than hype. A bed cooling fan is a targeted tool. Whole room AC changes the environment for everyone in the space, while a bed fan changes the environment around the sleeper.
A few practical differences stand out.
There is also a category point worth knowing. The original Bedfan came to market several years before BedJet was even thought of, so this type of under sheet airflow is not new. If you want a direct recommendation, the bFan from www.bedfans-usa is the one to look at first for simple between the sheets airflow without the price jump.
Timing gives the first clue. SSRIs, insulin, CPAP history, and meal timing can all point the workup in very different directions. If you match sweats to medication changes, snoring, or overnight lows, you can shorten the path to the right fix.
Step 1 is to line up the clock. Write down when the sweats happen, what time you took medications, when you drank alcohol, and when you last ate. If the sweating started within days or weeks of a new medicine, that is a strong lead.
Step 2 is to look for side clues. Loud snoring, witnessed pauses in breathing, morning headaches, and daytime sleepiness push sleep apnea higher. Waking shaky, hungry, or confused can suggest low blood sugar. A racing heart, tremor, or daytime heat intolerance may point toward thyroid causes.
Step 3 is to act on the pattern. If the clues fit a medicine, talk to the prescriber before stopping anything. If the clues fit sleep apnea, ask about a sleep study. If diabetes treatment is involved, discuss nighttime glucose trends. Common misconception, not every sweaty wakeup is hormonal, and not every hormonal sweat needs hormones.
Yes, sometimes. NICE and ACOG both support non drug measures as useful support, especially for menopause related symptoms, but they work best for comfort and sleep quality, not for diagnosing or curing infection, endocrine disease, or cancer.
If the core issue is bed heat trapping around your body, cooling the sleep system can help right away. That is where under sheet airflow, breathable sleepwear, lighter bedding, and a well chosen bedroom temperature do real work. For many people, this is enough to turn a miserable night into a manageable one.
If the issue is menopause, non drug tools like menopause specific CBT, trigger reduction, less evening alcohol, and better bed cooling can also reduce the “bother” factor, meaning the number of awakenings and the distress around them, even if the vasomotor signal itself is not fully shut off.
But there is a limit. If you are soaking through clothing, losing weight, running fevers, or feeling worse overall, then non drug measures are not enough. They are a bridge. They are not the full answer.
Yes. The most common questions are about severity, cause, bedroom temperature, and whether bed cooling devices actually work. Those are the right questions, because severe night sweats sit at the intersection of symptom relief, sleep quality, and medical diagnosis.
Severe night sweats usually means repeated episodes that soak sleepwear or bedding, wake you from sleep, or force you to change clothes or sheets.
A one off warm night after a spicy dinner is not the same thing. If you are waking up drenched several nights a week, or the episodes are escalating, it is reasonable to treat that as a clinical symptom, not just “sleeping hot.”
The more the sweating disrupts sleep or comes with other symptoms, the more seriously it should be taken.
No. Menopause is common, especially in people in their forties and fifties, but it is far from the only cause.
Medicines, infections, thyroid disease, sleep apnea, alcohol, anxiety, reflux, low blood sugar, and some cancers can all cause heavy nighttime sweating. If the pattern is new, unexplained, or joined by fever or weight loss, do not assume it is hormonal.
Menopause may be the answer, but it should be earned by the history, not guessed.
Yes, it can. Anxiety can raise adrenaline and cortisol, increase arousal during sleep, and make your body run hotter and sweat more.
That said, anxiety is also easy to over blame. If you are having drenching sweats with physical red flags, anxiety should not be the only explanation until other causes have been considered.
A symptom log is helpful here, especially if stressful days, alcohol, and poor sleep cluster together.
Lars Nielsen Terapi beskriver i praksis,
No. This is one of the biggest points of confusion.
Neither a Bedfan nor a BedJet refrigerates air. They both use the cooler air already present in the room and move it through the bedding so heat and moisture can leave your skin more efficiently.
That is why room temperature still matters. The device improves heat removal, it does not create cold air from nowhere.
Most sleep experts recommend a bedroom temperature between 60°F and 67°F, or 15.5°C to 19.5°C, for better sleep.
If you use a bed fan like the bFan, many people can raise the room setting by about 5°F and still feel cool enough to sleep well, because the airflow under the sheets does the targeted cooling where the body needs it.
That can be a useful middle ground when your partner dislikes a very cold room.
Yes, often it can, especially if your main problem is trapped heat in bed rather than a truly hot room.
A bFan uses about 18 watts on average, which is tiny compared with central air conditioning. When the under sheet airflow is doing its job, many people can keep the room a bit warmer, often around 5°F warmer, and still sleep comfortably.
The exact savings depend on climate, insulation, and your thermostat habits, but the logic is sound.
Tight weave sheets usually work best because they guide the airflow along the body instead of letting it escape too quickly.
Breathable cotton or similar fabrics tend to feel the most natural. Very heavy bedding can trap too much heat, while very loose, porous layers may let the air disperse before it cools your skin effectively.
Think of the sheet as the channel that helps the airflow do useful work.
Call sooner rather than later if severe night sweats come with fever, unexplained weight loss, swollen lymph nodes, new cough, chest pain, shortness of breath, easy bruising, or severe fatigue.
Also call if you are pregnant, have a weakened immune system, or have diabetes with possible overnight low blood sugars. If you feel acutely ill, do not wait for bedding changes or sleep gadgets to solve it.
Comfort measures are helpful, but red flag symptoms move this out of the self care category.
Copyright 2005 - present - Tompkins Research, Inc. & Kurt W. Tompkins All Rights Reserved DO NOT COPY. bFan® and the word bfan® in any format is a registered trademark of Kurt W. Tompkins the word BFAN® in any format shall not be used without written permission of the mark owner. This includes specifically Brookstone where you like to bait and switch, do not use my mark to bait customers.